How To Choose a HIPAA-Compliant Telehealth Platform for Your Healthcare Practice
Last updated:7 November 2025

Choosing the right telehealth platform isn’t easy. You’re balancing patient care, compliance, and technology while trying to keep your team confident and your data secure. Every click, every video call, and every shared file carries risk when protected health information is involved.
You already know HIPAA matters. What you need is clarity: what exactly makes a telehealth platform HIPAA compliant, which platforms truly meet those standards, and how to choose one that fits your practice without adding unnecessary complexity or cost.
In this guide, you’ll find clear answers. We’ll explain what HIPAA compliance means for telehealth, why it matters for your organization, what to look for in secure platforms, and how to set one up the right way. You’ll also see examples of trusted HIPAA-compliant telehealth platforms and learn how TechMagic can help you build or integrate a custom, compliant solution that fits your workflow.
Key Takeaways
- HIPAA compliance is the foundation of safe telehealth. It protects patient privacy, builds trust, and ensures your virtual care operations meet federal security and privacy standards.
- Not all telehealth platforms are created equal. Only HIPAA-compliant telehealth platforms that meet technical, administrative, and physical safeguard requirements can legally handle Protected Health Information (PHI).
- Compliance must be a culture. True compliance means combining secure technology with trained staff, documented policies, and ongoing risk assessments.
- Transparency drives patient trust. Clear communication about how you store and protect patient data reassures patients and improves engagement in virtual care.
- Choosing the right platform requires a balanced approach. Evaluate each solution for security, usability, scalability, and integration with existing systems like electronic health records and practice management tools.
- Implementation matters as much as selection. Even the most secure platform can fail if you skip key setup steps: signing a BAA, enabling encryption, limiting access, and training your team.
- Custom solutions offer lasting flexibility. Partnering with experts like TechMagic helps you build or integrate telehealth systems tailored to your workflows. This may be custom software or cost-effective Medplum-based development.
What HIPAA Compliance Means for Telehealth
HIPAA compliance in telehealth means protecting every piece of patient information before, during, and after a virtual visit. It ensures that the technology used to deliver care meets strict standards for privacy, security, and confidentiality.
For any telehealth platform to be truly HIPAA compliant, it must safeguard Protected Health Information (PHI) through both technical measures and organizational practices.

What is HIPAA, and its role in digital healthcare
The Health Insurance Portability and Accountability Act (HIPAA) was created to protect patients’ medical information and give them control over who can access it.
Initially built for paper records, it now extends deeply into the digital landscape, including telemedicine, remote monitoring, and patient portals. In this context, telehealth vendors often act as business associates, which means they’re legally bound to handle PHI responsibly and follow HIPAA standards.
How HIPAA applies to telehealth platforms
Telehealth tools process PHI every time a patient’s name, diagnosis, or lab result passes through a call or message. That means every chat, video session, or file transfer must happen in a secure, compliant environment.
A telehealth HIPAA compliant platform uses encryption, access control, and audit trails to make sure that data stays protected end to end. Vendors must also sign a business associate agreement (BAA) with healthcare providers: a legal promise to follow HIPAA rules.

Key Privacy Rule requirements for telehealth providers
The HIPAA Privacy Rule limits how patient data can be used and shared. In telehealth, that means only the minimum necessary information should be accessed, and only by authorized staff. Patients must give consent before any disclosure, and providers must clearly explain how their data is stored or shared, even for telehealth sessions.
Key Security Rule safeguards for telehealth platforms
HIPAA’s Security Rule focuses on how you protect electronic PHI (ePHI). It includes administrative, physical, and technical safeguards that work together to reduce risk and ensure confidentiality. Below are the key requirements they include.
Technical safeguards: core requirements for secure telehealth systems
- Access controls and user authentication. Only verified users should reach patient data.
- End-to-end encryption. Protects data during transmission and storage.
- Automatic logoff and session timeout. Prevents unauthorized access from idle sessions.
- Audit controls and activity monitoring. Tracks who accessed what and when.
- Data integrity and transmission security. Ensures information isn’t altered or lost in transit.
Administrative safeguards: policy and process compliance
- Workforce training and access management. Every staff member must understand and apply HIPAA principles.
- Business associate agreements (BAAs). Legal agreements that define each party’s responsibility.
- Risk analysis and ongoing security review. Regularly assess where vulnerabilities may exist.
- Contingency and incident response plans. Prepared responses for data loss or security events.
Physical safeguards: protecting data storage and access points
- Secure facility and device access. Limit entry to authorized personnel only.
- Mobile device management and secure disposal. Encrypt devices and erase PHI before disposal.
- Environmental protection for hardware. Safeguard equipment that stores or processes sensitive data.
Why HIPAA Compliance Matters in Telehealth
Compliance with HIPAA is the foundation of safe, trustworthy digital care. In telehealth, where clinical interactions rely entirely on technology, compliance protects both patients and providers. It ensures that data stays private, systems stay secure, and relationships stay grounded in confidence rather than risk.

Here are the key “whys”:
Patient trust depends on privacy and transparency
Every virtual visit starts with trust. Patients need to know their personal health information is protected just as securely as it would be in a physical clinic. When your telehealth system clearly communicates how data is used, stored, and shared, it strengthens confidence and encourages patients to speak openly, which leads to better care outcomes.
In 2023, the U.S. healthcare sector reported 725 large-scale data breaches, exposing more than 133 million patient records. This is the highest number on record. Such a level of exposure shows why patient confidence in virtual care depends on visible, enforceable privacy and security measures.

Non-compliance leads to costly penalties and reputational loss
The financial risk of violating HIPAA can be devastating. Fines range from thousands to millions of dollars, depending on the level of negligence. But beyond penalties, the real cost is reputational. One headline about a privacy breach can undo years of patient loyalty and hard-earned credibility.
The Office for Civil Rights (OCR) has already imposed $144.9 million in HIPAA violation settlements and penalties across 152 cases since enforcement began.
Data breaches undermine confidence in virtual care
A single security lapse, an unencrypted call, an exposed file, or an unsecured device can erode public trust. Once confidence in digital healthcare falters, adoption slows and patient engagement suffers. A telehealth HIPAA compliant platform helps prevent this as it secures every data exchange, every time.
Strong compliance differentiates providers in a competitive market
Telehealth adoption has accelerated, and patients now have options. Demonstrating strong compliance gives your organization an edge. It shows you take security seriously, which appeals not only to patients but also to partners, insurers, and enterprise clients evaluating which telehealth platforms are HIPAA compliant and reliable.
Secure systems ensure sustainable and resilient telehealth operations
To ensure HIPAA compliance means to be ready for tomorrow’s risks. When you build security into your telehealth infrastructure, you’re also investing in stability, scalability, and business continuity. Systems that are secure by design stay adaptable in a dynamic digital healthcare industry.
Protecting patient data is an ethical and professional obligation
Beyond policy, compliance reflects a core value of healthcare: do no harm. Protecting data is part of that promise. Upholding patient privacy in virtual care honors the same ethical commitment healthcare professionals make in person.
Real-world violations show the consequences of neglecting compliance
The Office for Civil Rights (OCR) regularly investigates breaches caused by unsecured video platforms, missing BAAs, or misconfigured cloud storage. These cases serve as reminders: even small oversights can lead to major fallout. Staying compliant means learning from these examples and building proactive safeguards.
Since 2003, OCR has resolved over 370,000 HIPAA-related complaints and required corrective action in more than 31,000 cases.
Key Factors to Consider When Choosing a Telehealth Platform
Choosing the right telehealth platform is a long-term investment in care quality, compliance, and trust. The best HIPAA-compliant telehealth platforms balance security and usability. Before making a decision, take time to evaluate these critical factors.
HIPAA and regulatory compliance readiness
Start with the basics: if a platform isn’t telehealth HIPAA compliant, it’s not an option. Verify that the vendor fully supports HIPAA’s Privacy and Security Rules, signs a business associate agreement (BAA), and provides clear documentation of compliance. If your organization also handles insurance billing, confirm readiness for related frameworks like HITECH and PCI DSS.
Data encryption, access control, and secure storage
A platform’s encryption standards reveal how seriously it treats data protection. Look for end-to-end encryption, strong password policies, and secure user authentication methods such as multifactor login. Ask whether PHI is stored in the cloud or on-premises, how it’s encrypted at rest, and whether data backups are also secured under HIPAA standards.
Business associate agreement and vendor accountability
A signed BAA is a HIPAA requirement. It defines the vendor’s legal obligation to safeguard patient data. Without it, your organization bears full liability for breaches. Ensure the vendor offers a detailed, up-to-date BAA and is transparent about how it manages third-party partners and subcontractors.
Clinical workflow compatibility and ease of use
Technology should simplify care, not slow it down. A good platform fits seamlessly into your clinicians’ daily routines. During demos, involve your care team to test usability. If it takes more than a few clicks to start a call or record a note, adoption will drop.

EHR and practice management system integration
Integration is what turns a telehealth platform into a complete care solution. Look for native or API-based connections with your EHR, billing, and scheduling systems. Integration minimizes manual entry, reduces errors, and supports consistent documentation, essential for compliance and reporting.
Support for multi-specialty and cross-department use
A telehealth platform must adapt to different clinical contexts. Behavioral health, primary care, and rehabilitation all have unique needs. Choose a platform flexible enough to handle different session types, templates, and patient engagement tools without requiring separate systems.
Video and communication quality under real-world conditions
Even the most secure platform fails if the video freezes or audio drops mid-consultation. Test for quality and latency under typical network conditions. Providers working in rural or bandwidth-limited areas should confirm that the system automatically adjusts video resolution without compromising stability.
Scalability and cloud infrastructure reliability
As telehealth volumes grow, your platform must scale easily. Ask vendors about uptime guarantees (99.9% is a good benchmark), disaster recovery plans, and load-handling capacity. Cloud-based systems usually scale faster and support remote updates. But confirm the hosting environment is certified for healthcare data.
Customization and white-labeling capabilities
Custom branding and flexible workflows help maintain a consistent patient experience. White-label options allow organizations to use their own logo, colors, and communication templates while keeping the backend secure and compliant. This is particularly useful for multi-location networks and telehealth startups.
Interoperability with healthcare standards (HL7, FHIR, APIs)
Interoperability is the backbone of modern healthcare IT. Choose a platform that supports HL7 and FHIR standards for data exchange. These allow secure messaging and communication between systems like labs, pharmacies, and hospitals.
User experience for patients and providers
A telehealth system must work for everyone. Look for intuitive interfaces, minimal clicks, and clear prompts. Patients should be able to join a session without extra downloads or technical hurdles. Providers should have quick access to records, notes, and follow-ups during the call.
Accessibility and mobile device optimization
Accessibility means inclusivity. Ensure the platform meets WCAG accessibility standards and runs smoothly on mobile devices, tablets, and desktops. Features like closed captioning, screen-reader support, and adaptable interfaces make care accessible to a wider audience.
Vendor security certifications and compliance audits
Trust is earned through transparency. Reputable vendors undergo independent audits and maintain certifications such as SOC 2, ISO 27001, or HITRUST. Ask for proof of recent compliance audits, penetration test results, and documentation of how they address vulnerabilities.
Technical support and service-level agreements (SLAs)
Reliable support can make or break your telehealth operations. Evaluate the vendor’s response times, 24/7 support options, and escalation procedures. A clear SLA should specify uptime guarantees, incident response timelines, and support channels for emergencies.
Total cost of ownership and ROI for your practice
Upfront pricing rarely tells the full story. Consider setup fees, training costs, BAA coverage, integration expenses, and future upgrades. A slightly higher initial cost may deliver better ROI if it reduces downtime or improves patient satisfaction. Ask vendors for transparent pricing and real-world case examples.
Long-term product roadmap and innovation potential
Telehealth technology is evolving fast. Choose a partner, not just a platform. Ask vendors about upcoming features: AI-assisted documentation, analytics dashboards, or new API integrations. A clear product roadmap signals long-term commitment and alignment with your digital health strategy.
The right HIPAA compliant platforms for telehealth are built to last. Evaluating the abovementioned factors helps you choose a system that protects patient data, supports clinicians, and scales with your organization’s growth.

Top Examples of HIPAA-Compliant Telehealth Platforms
The telehealth market offers a range of secure, compliant video conferencing tools built for different types of practices and patient needs. Choosing the right telehealth option depends on your size, specialty, workflow, and how much customization you require.
Below are some of the most trusted HIPAA-compliant telehealth platforms, along with what makes each one stand out.
Doxy.me – Simplicity and accessibility for small practices

Doxy.me is a web browser-based platform known for its simplicity. There’s nothing to download, and patients can join sessions with a single click. Its free plan offers basic encrypted video, while paid versions include branding and virtual waiting-room features.
Best for: solo practitioners and small clinics looking for an affordable, no-fuss way to provide HIPAA-compliant video visits.
Key strengths: ease of use, no installation required, quick setup, and reliable security with end-to-end encryption.
Zoom for Healthcare – Enterprise-level video with HIPAA compliance
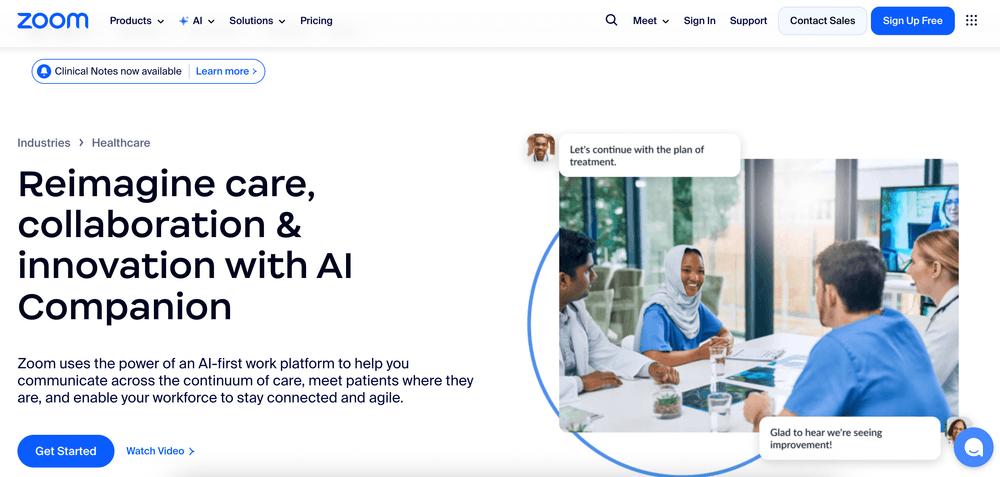
Zoom for Healthcare builds on Zoom’s familiar interface but includes enhanced security and compliance features. It supports BAAs, AES 256-bit encryption, and integration with leading EHRs such as Epic and Cerner. The platform scales well for large organizations running multiple concurrent sessions.
Best for: hospitals, enterprise healthcare networks, and academic medical centers that need scalable video communication.
Key strengths: high-quality video, strong compliance documentation, enterprise integration, and customizable workflows.
VSee – Flexible Platform for Startups and Specialty Clinics
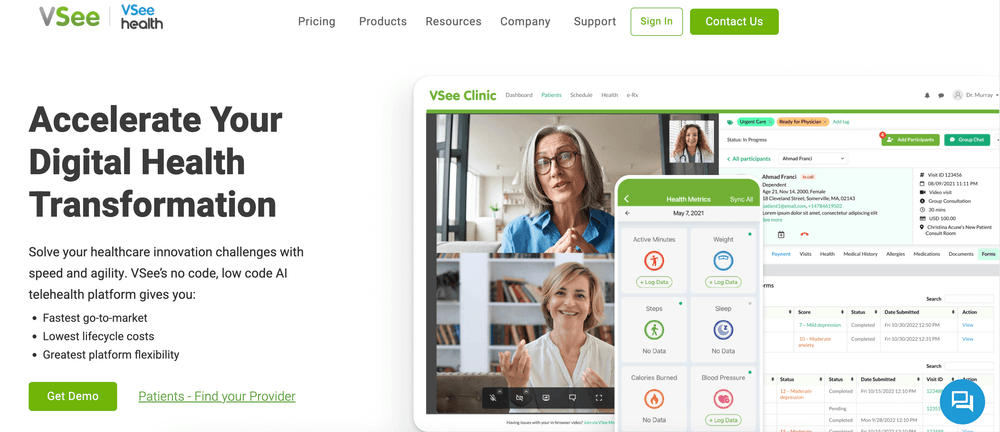
VSee offers modular HIPAA-compliant telehealth tools, including video visits, remote monitoring, and patient triage. It’s known for flexibility, which makes it a strong option for startups or specialty providers who want to tailor workflows without building from scratch.
Best for: niche healthcare startups or specialty practices (like behavioral health or dermatology) that value agility and customization.
Key strengths: modular design, medical device integration, API flexibility, and HIPAA-ready infrastructure.
Mend – All-in-one telehealth and patient engagement solution
Mend has more than just video calls. It offers automated appointment reminders, digital intake forms, and real-time analytics. It’s designed to reduce no-shows and improve patient engagement through automation.
Best for: multi-provider practices or clinics seeking an integrated patient communication suite.
Key strengths: comprehensive engagement tools, user-friendly design, EHR integrations, and advanced analytics for operational insight.
SimplePractice – Integrated practice management for therapists and counselors
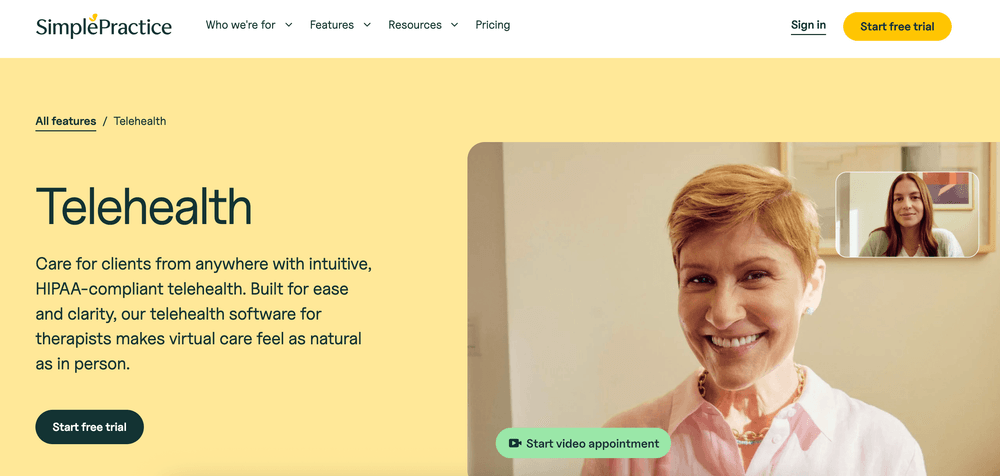
SimplePractice combines telehealth with practice management: scheduling, billing, and documentation all in one place. It’s particularly popular among mental health professionals who value simplicity and security.
Best for: therapists, psychologists, and counselors running private practices or small group practices.
Key strengths: seamless scheduling, note templates, secure video, and easy client onboarding through a patient portal.
Teladoc Health – Scalable virtual care network for large organizations
Teladoc Health is one of the most established virtual care networks globally. It offers end-to-end telehealth infrastructure, clinical staffing, and AI-driven triage systems. Designed for enterprise-scale delivery, it’s a fully HIPAA-compliant telehealth software and trusted by major healthcare systems.
Best for: large health systems, insurers, and organizations looking for global reach and advanced telehealth analytics.
Key strengths: scalability, global infrastructure, deep analytics, and extensive compliance support.
Amwell – Robust platform for hospitals and health systems
Amwell provides a comprehensive virtual care ecosystem with EHR integration, white-label options, and secure communication tools. It’s used by top U.S. hospital systems to connect patients, clinicians, and specialists through a unified telehealth experience.
Best for: hospitals and integrated delivery networks that require enterprise-level reliability.
Key strengths: strong EHR integration, customizable modules, patient triage capabilities, and proven compliance with HIPAA.
Custom telehealth solutions and integrations with TechMagic
Sometimes, off-the-shelf platforms don’t fully fit your needs, especially if you’re managing complex workflows, multi-system integrations, or a unique patient experience. That’s where we can help.
Our team builds and integrates custom telehealth HIPAA compliant platforms designed around your organization’s goals.
If you need to connect existing systems, extend features, or create a tailored interface for your clinicians and patients, we make it secure, scalable, and easy to maintain.
We also specialize in Medplum development, a cost-effective, open-source foundation for healthcare applications. With Medplum, we can accelerate custom development, ensuring compliance, interoperability, and long-term flexibility.
If you’re considering building your own solution instead of using an existing one, learn more about the process and best practices in our guide to HIPAA compliant app development.
Best for: organizations seeking a telehealth platform designed precisely around their workflow and security needs.
Key strengths: HIPAA compliance by design, seamless integrations, Medplum-based cost efficiency, and deep healthcare software expertise.
Learn about our expertise in the industry and what we have to offer

Each of these telehealth platforms HIPAA compliant options meets the technical standards for security but the right choice depends on your size, specialty, and long-term strategy.
Best Practices for Setting Up a HIPAA-Compliant Telehealth System
Once you’ve chosen a platform, compliance doesn’t stop there. How you configure, monitor, and maintain your system determines if it truly stays HIPAA compliant. The goal is to create a telehealth environment that is secure by design. Here’s how to achieve it.
Conduct a comprehensive risk assessment before deployment
Before launching any telehealth service, evaluate every possible vulnerability. Map how protected health information (PHI) flows through your system. Identify potential weak points like unsecured devices or cloud misconfigurations. A formal risk assessment not only meets HIPAA guidelines and requirements but also helps you prioritize fixes before issues become breaches.
Configure secure access controls and user authentication
Access control is your first line of defense. Limit user access to only what’s necessary for their role. Use unique credentials, strong passwords, and multi-factor authentication for both staff and administrators. Disable generic logins or shared accounts. They're one of the most common sources of unauthorized access in healthcare systems.
Enable end-to-end encryption and secure data storage
Encryption protects data everywhere it travels. Make sure your platform uses end-to-end encryption for video, chat, and file transfers. Data should also be encrypted “at rest” in databases or cloud storage. If your platform stores session recordings or attachments, confirm they’re encrypted and access-restricted by default.

Implement role-based permissions and activity auditing
Every click that touches patient data should be traceable. Role-based access ensures users only see what they need and nothing more. Audit logs should track logins, file downloads, and configuration changes. Review them regularly to catch anomalies early and document compliance for potential audits.
Train staff on HIPAA policies and secure virtual communication
Technology is only as secure as the people who use it. Regular training helps staff recognize phishing attempts, handle PHI correctly, and use telehealth tools responsibly. Include refreshers whenever systems update or new features launch. Empower your team to report security concerns quickly and without fear.
Establish data backup, retention, and disaster recovery procedures
Data loss can be just as damaging as a breach. Implement automated, encrypted backups stored in HIPAA-compliant environments. Test your recovery plan regularly to ensure you can restore critical data quickly after an outage or cyberattack. Define retention periods that comply with both HIPAA and your state’s medical record laws.
Common Mistakes to Avoid When Choosing Telehealth Platforms
Even the best telehealth platform can fail to stay compliant if it’s used carelessly. Knowing these pitfalls early helps you prevent them before they become costly problems.
Choosing a non-HIPAA-compliant platform or consumer app
It might seem convenient to use tools your staff already knows, like FaceTime or WhatsApp, but most consumer-grade apps don’t meet HIPAA standards. They lack business associate agreements, strong encryption, and access controls. Even one unprotected session can qualify as a HIPAA violation.
How to prevent it: Always verify that your provider offers a signed BAA, HIPAA-compliant encryption, and data-handling documentation. Never assume compliance because a platform “feels” secure.
Ignoring security configuration after platform setup
Many organizations install secure platforms but never adjust the default settings. Leaving open ports, weak passwords, or unused accounts is like locking the door but leaving the window open.
How to prevent it: After setup, conduct a full configuration audit. Disable unused features, enforce multi-factor authentication, and apply role-based permissions. Schedule regular system checks to ensure configurations remain intact after updates.
Neglecting integration with EHR and existing clinical workflows
When telehealth platforms operate in isolation, staff often copy and paste data between systems. This increases the risk of exposure and mistakes. Manual data handling also slows down care delivery.
How to prevent it: Choose a solution that integrates directly with your EHR or practice management system through FHIR or HL7 APIs. Seamless integration keeps PHI contained within secure systems and simplifies documentation.
Get Your Reliable Partner in HIPAA-Compliant Telehealth Solutions
Building a secure, reliable telehealth experience takes more than software. It takes a partner who understands both technology and healthcare. That’s where TechMagic can help.
We help healthcare organizations design, build, and integrate HIPAA-compliant telehealth platforms that meet today’s strict security standards while staying flexible for tomorrow’s innovation.
Our approach starts with understanding your workflows, compliance needs, and patient experience goals. If you need to develop a platform from the ground up or integrate telehealth into your existing system, we ensure every solution aligns with HIPAA, HITECH, and interoperability standards like FHIR and HL7.
For organizations looking to move faster and more cost-effectively, we offer development based on Medplum, an open-source healthcare platform that provides a secure, API-first foundation for digital health applications. Medplum helps reduce time-to-market, cut infrastructure costs, and maintain full HIPAA compliance without sacrificing performance or customization.
TechMagic has helped startups, clinics, and enterprise healthcare providers modernize care delivery with scalable, compliant digital tools.
We deliver HIPAA-compliant:
- Telehealth platforms that ensure secure, seamless, and scalable virtual care delivery.
- Custom healthcare software solutions designed around your unique workflows and data needs.
- EHR/EMR systems focused on interoperability, usability, and intuitive design.
- HIPAA compliance consulting services providing end-to-end support to help you achieve and maintain HIPAA compliance.
If you’re ready to create or enhance your telehealth solution securely and efficiently, our team is here to help. Let’s build something that empowers your clinicians, protects your patients, and strengthens your practice.

Wrapping Up: Building a Secure and Future-Ready Telehealth Practice
Compliance with HIPAA is what makes telehealth credible, safe, and sustainable. By now, you know what HIPAA-compliant telehealth platforms are, why they matter, and how to choose and set up one correctly. You’ve seen real examples, common pitfalls to avoid, and best practices that help your team stay secure and confident.
If your current telehealth system feels limited, outdated, or fragmented, this is the right time to rethink your approach. If you’re integrating an existing platform or building one tailored to your organization, TechMagic can help you do it securely, efficiently, and with patient trust at the center of every click.
Looking ahead, telehealth will only grow more intelligent, connected, and personalized. We’ll see AI-driven triage, real-time health data from wearables, and deeper EHR interoperability becoming the new normal.
As technology advances, so will regulatory expectations. HIPAA compliance will remain a constant anchor amid rapid innovation. Practices that invest in secure, flexible infrastructure today will be best positioned to adapt tomorrow while offering care that’s both compliant and genuinely patient-centered.
FAQ

A telehealth platform is HIPAA compliant when it meets all HIPAA Privacy and Security Rule requirements, including encryption, access controls, audit logs, secure data storage, and a signed business associate agreement (BAA) with the vendor.
No. Many general-purpose video apps and telehealth remote communication tools don’t meet HIPAA standards or offer BAAs. Always check if it is a HIPAA-compliant telemedicine platform before using it and exchanging and storing patient information.
Compliance protects patient data, prevents costly penalties, and builds trust. It also ensures your organization can safely scale and provide telehealth services without risking privacy violations.
Look for end-to-end encryption, secure authentication, audit logs, and seamless EHR integration. Reliable vendors will also sign a BAA and provide documentation proving their compliance measures.
HIPAA-compliant telehealth platforms are virtual care solutions that follow HIPAA standards to protect patient information during online consultations. These platforms use secure encryption, restricted access, and data management controls to ensure all communications and records remain confidential and compliant.
Platforms like Doxyme, Zoom for Healthcare, VSee, Mend, SimplePractice, Teladoc Health, and Amwell are recognized as telehealth platforms HIPAA compliant for different practice sizes and needs. You can also build a custom HIPAA compliant platform for telehealth with TechMagic for full flexibility and control.

















 TechMagic Academy
TechMagic Academy





